
How to Fix Cracked Heels Permanently: Home Care + Professional Treatment
Cracked heels look small on the surface, but they can change how you stand, walk, and move through your day. When fissures deepen, every step

Medically Reviewed by
Dr. Peter Hanna, DPM
Board Certified Podiatrist

Ankle injuries are among the most common musculoskeletal problems in the United States, affecting athletes, weekend warriors, and everyday individuals alike. An estimated 25,000 Americans sprain an ankle every single day and that figure does not even account for fractures, ligament tears, tendon ruptures, and syndesmotic injuries that send patients to emergency departments across the country. In South Florida, where outdoor activities, water sports, and an active lifestyle are part of the culture, ankle injuries are especially prevalent.
At South Florida Multispecialty Medical Group (SFL Medical Group), our podiatry and sports medicine teams diagnose and treat a full spectrum of ankle injuries every day. Whether you rolled your ankle on the beach or heard a pop during your morning run, understanding the type of injury you are dealing with is the first step toward a full recovery.
The ankle is a highly complex joint. It connects three major bones the tibia (shinbone), fibula (outer bone of the lower leg), and talus (ankle bone) and relies on a network of ligaments, tendons, and muscles to maintain stability and function. Every time we walk, run, jump, or pivot, enormous forces pass through this joint.
When those forces exceed what the surrounding structures can handle, whether from a sudden twist, direct trauma, or cumulative overuse, an injury occurs. The type of injury depends on the mechanism of force, the structures involved, and the degree of damage sustained.
Understanding the anatomy helps us match the injury to the right treatment. A lateral sprain affecting the outer ligaments requires a very different approach than a bimalleolar fracture or a syndesmotic tear. Let us break down each major type of ankle injury in detail.
Ankle sprains account for nearly 40% of sports-related injuries reported in emergency departments nationwide. A sprain occurs when the ligaments supporting the ankle are overstretched or torn due to a sudden twisting or rolling motion. The most frequent mechanism is the foot rolling inward (inversion) while the ankle turns outward, a motion many of us have experienced when stepping off a curb unexpectedly or landing awkwardly from a jump.
Lateral ankle sprains, involving the ligaments on the outside of the ankle, are by far the most common type. The medial side (inner ankle) is far less frequently injured because the deltoid ligament complex on that side is considerably stronger. However, when medial sprains do occur, they often accompany severe trauma or fractures.

Not all sprains are the same. Clinicians classify ankle sprains into three grades based on severity:
A Grade I sprain involves mild stretching of the ligament fibers with microscopic tearing. The ankle remains structurally stable. Swelling and tenderness are present but mild, and most patients can still bear weight, though with some discomfort. Recovery typically takes two to four weeks with proper rest and care.
The ligament is partially torn. Swelling and bruising appear more prominently, and patients often notice moderate instability in the joint. Walking becomes painful, and bearing full weight may not be possible in the initial days. Recovery takes approximately four to eight weeks depending on the extent of the tear and the rehabilitation protocol followed.
This is a complete tear of the affected ligament. The joint becomes significantly unstable, and patients frequently report feeling or hearing a “pop” at the moment of injury. Severe swelling, bruising, and an inability to walk normally are classic signs. Grade III sprains often require bracing or casting, and in some cases surgical repair. Recovery can extend from three to six months or longer.

The lateral ligament complex consists of three bands:
On the medial side, the deltoid ligament provides strong resistance to eversion forces. Isolated medial sprains are uncommon and usually only occur alongside fractures or high-energy trauma.
A high ankle sprain is a distinctly different injury from a typical lateral ankle sprain, and it is often more serious. This injury affects the syndesmosis, the band of ligaments that connects the tibia and fibula just above the ankle joint. The mechanism typically involves forced dorsiflexion combined with external rotation, a movement common in contact sports like football, hockey, and soccer.
What makes high ankle sprains particularly tricky is their location. Pain is felt higher than in a standard ankle sprain, along the front and sides of the lower leg rather than at the outer ankle. Swelling extends above the ankle, and walking, climbing stairs, or any weight-bearing activity tends to aggravate symptoms significantly.
Recovery from a high ankle sprain often takes twice as long as a standard ankle sprain. Grade I and II syndesmotic sprains are typically managed conservatively with immobilization, crutches, bracing, and a structured physical therapy program. Grade III injuries, those involving complete syndesmotic disruption or diastasis (widening of the gap between the tibia and fibula), often require surgical stabilization using screws or suture-based fixation devices to restore proper alignment.
If a high ankle sprain is misdiagnosed as a routine lateral sprain and treated insufficiently, patients frequently develop chronic pain, instability, and early onset joint damage. At SFL Medical Group, we use advanced imaging and clinical stress tests to accurately diagnose syndesmotic injuries and prevent these long-term complications.
An ankle fracture is a break in one or more of the bones forming the ankle joint: the tibia, fibula, or talus. Fractures can occur from high-impact trauma such as falls, car accidents, or severe sports injuries. However, they also result from twisting injuries that are initially mistaken for sprains.
One of the most important clinical facts about ankle fractures: you might still be able to walk. Many patients assume that if they can put weight on an ankle, nothing is broken. That assumption is dangerous. Imaging, specifically X-rays and sometimes CT scans, is essential whenever ankle pain persists following an injury, or when the Ottawa Ankle Rules criteria are met during a physical examination.

This is the most common type of ankle fracture. It involves the distal end of the fibula, the bony bump on the outer ankle. Twisting injuries, falls, or inversion trauma are the usual causes. Stable, non-displaced lateral malleolus fractures can often be treated conservatively with a walking boot and activity restriction. Displaced fractures may require surgical fixation.
The medial malleolus is the inner bony prominence of the tibia. Fractures here result from severe force or direct trauma to the inside of the ankle. These injuries frequently occur alongside lateral malleolus fractures in high-energy trauma scenarios.
A bimalleolar fracture involves both the lateral and medial malleoli simultaneously. This typically results from higher-energy mechanisms such as violent twisting, falls from height, or motor vehicle collisions. Because both sides of the ankle are compromised, the joint becomes significantly unstable, and surgical fixation is often required.
This is among the most severe ankle fractures, involving the lateral malleolus, medial malleolus, and the posterior portion of the tibia (posterior malleolus) all at once. The ankle joint becomes highly unstable and almost always requires surgical intervention to restore alignment and function.
A pilon fracture occurs when the weight-bearing surface of the tibia is crushed or shattered, often from axial loading injuries such as falling from a significant height and landing on the feet. These are complex, high-energy fractures requiring specialized surgical management and lengthy rehabilitation.
Clinicians frequently use the Danis-Weber classification to guide treatment decisions for ankle fractures. This system categorizes fibula fractures based on their location relative to the syndesmosis:
Understanding fracture classification guides our team at SFL Medical Group in recommending the most appropriate treatment pathway for each individual patient.
Ligament tears encompass a broader spectrum of soft tissue injuries around the ankle. While Grade III sprains represent the most severe form of ligament sprains, distinct ligament tears, particularly those involving multi-ligament complexes, carry unique challenges and treatment considerations.
The distinction between a sprain and a tear is important. A sprain involves overstretched or partially torn fibers. A tear implies a more severe injury, often a complete rupture. In the ankle, the most clinically significant complete tears involve the lateral ligament complex (ATFL and CFL together), the deltoid ligament, or the syndesmotic complex.
Multi-ligament injuries, though less common, require a thorough diagnostic workup. MRI remains the gold standard for evaluating soft tissue integrity, while clinical stress tests such as the anterior drawer test and talar tilt test provide important functional information during the physical examination. According to the NIH / NCBI StatPearls resource on acute ankle sprains, accurate grading and stress testing are essential for guiding appropriate care.
When ligament tears fail to heal correctly or when chronic instability develops after repeated sprains, surgical reconstruction may be necessary. Lateral ankle ligament reconstruction (such as the Brostrom procedure) is a well-established surgical technique used to restore stability and prevent ongoing joint damage.
While not a ligament injury, Achilles tendon injuries are among the most serious ankle-related conditions we treat. The Achilles tendon is the largest and strongest tendon in the human body, connecting the calf muscles to the heel bone. It plays an essential role in every step, sprint, and jump.
Achilles tendinitis involves inflammation and degeneration of the tendon due to overuse or repetitive stress. It typically presents as a dull, aching pain at the back of the ankle, particularly during or after physical activity.
An Achilles tendon rupture is a far more dramatic injury. It usually occurs during explosive movements such as a sudden sprint, a deep lunge, or a misjudged jump. Patients often describe feeling as though they were “kicked” or “shot” in the back of the ankle, followed immediately by significant weakness and an inability to push off through the foot. A palpable “pop” at the moment of injury is a classic hallmark.
Treatment for an Achilles rupture depends on age, activity level, and the severity of the tear. According to the Mayo Clinic, surgical repair is often preferred for younger, more active patients seeking a return to high-performance sport. Non-surgical functional bracing offers comparable long-term outcomes for less active individuals when combined with a structured rehabilitation program. Most patients can expect to resume daily activities within three to four months, with full athletic return typically requiring six to nine months of dedicated rehabilitation.
One of the most significant long-term complications of untreated or poorly managed ankle injuries is post-traumatic ankle arthritis. Research estimates that up to 80% of ankle arthritis cases develop as a direct consequence of previous trauma, particularly ankle fractures and repeated sprains that were not properly rehabilitated.
When ligaments fail to heal completely, the joint develops chronic instability. Over time, this abnormal movement causes cartilage breakdown, inflammation, and structural changes in the joint surfaces. Patients experience progressive pain, stiffness, and reduced mobility, often years after the original injury.
Early, appropriate treatment of ankle injuries is the most effective strategy for preventing arthritis. At SFL Medical Group, we emphasize proper rehabilitation to restore joint mechanics and reduce the cumulative stress that predisposes patients to this chronic condition.
Accurate diagnosis is the foundation of effective treatment. Our clinical team uses a combination of physical examination techniques and advanced imaging to evaluate every ankle injury thoroughly.
We evaluate swelling, bruising, tenderness to palpation, range of motion, and joint stability. Specific tests, including the anterior drawer test, talar tilt test, and squeeze test for syndesmotic injuries, provide critical information about which structures are involved and to what degree. The American Academy of Orthopaedic Surgeons (AAOS) recommends a thorough clinical assessment as the first step in any ankle sprain evaluation.
X-rays are the first-line imaging tool for ruling out fractures. When soft tissue assessment is needed, MRI offers detailed visualization of ligament integrity, tendon condition, and cartilage health. CT scans provide three-dimensional imaging for complex fractures requiring surgical planning. Diagnostic ultrasound offers a real-time, dynamic view of tendon and ligament structures, particularly useful for identifying partial tears.
Our treatment philosophy centers on individualized care. No two ankle injuries are identical, and our team tailors every treatment plan to the patient’s specific injury, lifestyle, and recovery goals.
For most Grade I and Grade II sprains, stable fractures, and mild to moderate ligament injuries, conservative treatment provides excellent outcomes:
For chronic or complex injuries, we offer advanced options including:
Surgery becomes necessary for Grade III ligament tears with persistent instability, displaced or unstable fractures, complete Achilles tendon ruptures in appropriate candidates, and injuries unresponsive to conservative care. Common procedures include:

Prevention is always preferable to treatment. Several evidence-based strategies significantly reduce the risk of ankle injuries for patients of all activity levels:
If you are active in sports or simply want to protect your ankle health for the long term, our sports medicine team at SFL Medical Group offers comprehensive injury prevention assessments and sport-specific conditioning programs.
Some ankle injuries can be monitored at home initially, but several warning signs demand prompt professional evaluation:
Delaying care when these signs are present risks improper healing, chronic instability, nerve or vascular damage, and accelerated joint degeneration. Our team at South Florida Multispecialty Medical Group provides same-day evaluations for acute ankle injuries and comprehensive management from initial diagnosis through full return to activity.
If you are experiencing ankle pain or suspect an injury, contact SFL Medical Group today and let our specialists get you on the path to recovery.

Dr. Peter Hanna is a board-certified podiatrist and reconstructive foot & ankle surgeon with over 15 years of experience. He serves as Director of Podiatry at South Florida Multispecialty Medical Group, specializing in complex reconstruction, minimally invasive surgery, and diabetic foot care.
Trust & Transparency: Editorial Policy | Contact Us
More To Explore

Cracked heels look small on the surface, but they can change how you stand, walk, and move through your day. When fissures deepen, every step
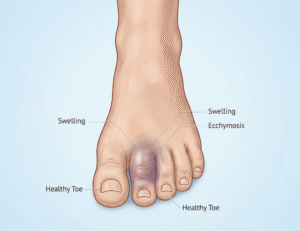
Roughly 8 to 10 percent of all fractures treated in emergency departments involve the foot and toes, yet a significant number of patients walk

©2026 South Florida Multispecialty Medical Group. All Rights Reserved.