
AOD-9604 Peptide: What It Is, How It Works, and What to Expect
What Exactly Is AOD-9604? Weight loss science has come a long way from appetite suppressants and crash diets. AOD-9604 represents one of the most targeted

Medically Reviewed by
Dr. Peter Hanna, DPM
Board Certified Podiatrist

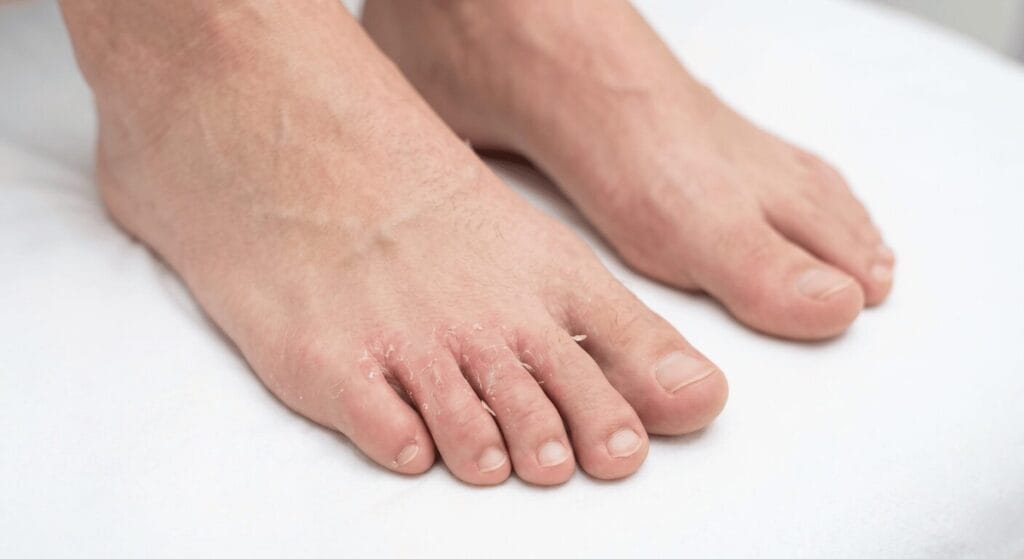
Most people associate athlete’s foot with an itchy, flaky rash between the toes. It is annoying, uncomfortable, and admittedly quite common but it stays on the feet, right? Not necessarily. Athlete’s foot, medically known as tinea pedis, is caused by dermatophyte fungi that actively feed on keratin, the protein found throughout our skin, hair, and nails. These organisms do not respect anatomical boundaries, and when given the right opportunity, particularly through hand contact or contaminated surfaces, they absolutely can spread beyond the feet.
One of the most surprising places they can travel? The face.
If you are wondering whether athlete’s foot can spread to your face, the answer is yes, though it requires a specific chain of events to get there. Understanding how this happens, what it looks like, and how to stop it in its tracks is exactly what we want to break down for you here.
Tinea pedis is a fungal infection caused primarily by Trichophyton rubrum and Trichophyton interdigitale. These dermatophytes thrive in warm, moist environments, think locker rooms, public showers, sweaty shoes, and damp socks. The infection typically begins between the toes and can extend to the soles, heels, and sides of the feet if left untreated.
Classic symptoms include:
Athlete’s foot is extraordinarily contagious. It spreads through direct skin-to-skin contact and through indirect contact with contaminated surfaces like floors, towels, shoes, and socks. You do not have to be an athlete to develop it, you simply need the wrong environment and a brief window of exposure.

Here is where the biology gets important. Dermatophyte fungi do not stay put once they take hold. If you scratch, pick, or rub the infected skin on your feet, which most people with athlete’s foot do instinctively, fungal spores transfer directly onto your hands. From there, those spores can be introduced to virtually any part of the body with sufficient warmth and skin surface.
The most common pathways for spreading include:
Contaminated clothing, bedding, and shared towels also serve as indirect vehicles for spreading the infection to new areas of the body and to other people in the household.
Yes and the medical term for it is tinea faciei. Facial fungal infections caused by dermatophytes are well-documented in clinical literature. Trichophyton rubrum, the primary culprit behind most cases of athlete’s foot, is one of the most frequently identified organisms in tinea faciei as well. The infection often traces its origin back to tinea pedis or tinea unguium (nail fungus) in the same patient.
The spread mechanism is usually auto-inoculation, which means you transfer the fungus from one part of your own body to another. For the face, this typically happens when a person:

Tinea faciei is more common than many people realize, yet it is also one of the most frequently misdiagnosed conditions in dermatology. Because the face has different skin characteristics than the feet, the infection often presents without the classic ring-shaped rash. Instead, it can appear as a red, slightly scaly, and irregularly shaped patch that mimics other conditions like rosacea, lupus, eczema, or contact dermatitis. Patients are sometimes treated for these conditions for weeks or months before the true fungal cause is identified.
Recognizing tinea faciei is genuinely tricky because the face responds differently to fungal infections than other skin sites. The presentation is often subtle at first and can worsen significantly when topical corticosteroids are mistakenly applied, a phenomenon known as “tinea incognito,” where anti-inflammatory creams mask the true nature of the infection while allowing the fungus to proliferate unchecked.
One pattern we consistently observe is that patients often report the facial rash appeared shortly after a flare-up of athlete’s foot or after scratching their feet. That chronological connection is a critical diagnostic clue. If you or a loved one develop a persistent, unexplained facial rash alongside a foot fungal infection, always mention both to your provider.
While athlete’s foot can affect anyone, certain individuals carry a notably higher risk of developing secondary infections that spread to the face or other body sites:
People living with conditions like HIV/AIDS, undergoing chemotherapy, or taking immunosuppressive medications have a reduced ability to mount a proper defense against fungal pathogens. In these cases, dermatophyte infections can be more aggressive, more widespread, and more resistant to standard treatments.
Diabetes alters circulation, immune response, and skin integrity. Diabetic patients are at elevated risk for both primary athlete’s foot and secondary spread. Fungal infections in diabetic individuals also carry the added concern of complications such as cellulitis, ulcerations, and in severe cases, limb-threatening infections, which is why early and comprehensive diabetic foot care is so important.
Athletes, military personnel, people who frequent communal locker rooms or pools, and anyone who wears occlusive footwear for prolonged periods face greater baseline exposure. Add habits like shared towels or not washing hands after touching the feet, and the risk of spreading the infection multiplies considerably.
Tinea faciei is particularly prevalent in children, often acquired from household pets carrying zoophilic fungi like Microsporum canis (from cats and dogs) or from close contact with infected family members. Children tend to touch their faces more frequently and are less consistent about hand hygiene. If your child is experiencing recurring foot or skin issues, our pediatric foot care team is here to help.
Accurate diagnosis is essential because treating fungal facial infections with the wrong medication especially topical corticosteroids, makes the condition significantly worse. A dermatologist or podiatrist familiar with fungal skin conditions will typically approach diagnosis through:
We strongly recommend against self-diagnosing facial rashes and applying over-the-counter hydrocortisone creams without a confirmed diagnosis. This is one of the most common errors we see, and it consistently delays proper treatment by weeks.
The good news is that tinea faciei responds well to antifungal treatment when properly diagnosed. The approach mirrors general tinea management but requires attention to the simultaneous treatment of the original source, the feet, to prevent reinfection.
For localized tinea faciei, topical antifungal creams remain the first-line option. Facial skin is more sensitive and thinner than other areas, so the choice of formulation matters. Commonly used agents include:
Treatment must continue for at least two weeks after symptoms resolve. Stopping early, even when the skin looks clear, is one of the most common reasons for recurrence.

When topical agents fail, when the infection is extensive, or when the patient is immunocompromised, oral antifungal therapy becomes necessary. Standard options include:
Oral antifungals require monitoring, particularly liver function testing in long-term regimens. These should always be prescribed and supervised by a licensed medical professional. According to StatPearls via the National Institutes of Health (NIH), topical imidazoles such as clotrimazole and ketoconazole offer effective remedies with a very low incidence of adverse effects for tinea infections.
Any treatment plan for tinea faciei must include simultaneous, aggressive management of athlete’s foot. Without clearing the source infection, reinfection of the face is almost inevitable. This means consistent application of antifungal treatments to the feet, maintaining excellent foot hygiene, and keeping footwear clean and dry throughout the treatment period. Our team offers comprehensive athlete’s foot treatment in Miami to help you eliminate the source infection completely.
Preventing the spread of athlete’s foot to the face and to other people comes down to a combination of hygiene discipline and environmental awareness. These strategies are not complicated, but consistency is everything:
Treating athlete’s foot promptly and completely is the single most effective way to prevent it from spreading. The longer an untreated infection persists on the feet, the higher the fungal load, and the greater the opportunity for auto-inoculation to the face, hands, groin, or nails. The Centers for Disease Control and Prevention (CDC) recommends keeping feet clean, dry, and cool, and wearing sandals in communal areas to minimize the risk of fungal spread. Do not wait until symptoms become severe. Early intervention saves time, discomfort, and the risk of complications.
Most mild cases of athlete’s foot respond to over-the-counter antifungal treatments. However, certain situations call for professional medical evaluation:
Our team at South Florida Multispecialty Medical Group provides comprehensive podiatry and dermatology services designed to diagnose and treat fungal infections at every stage. Whether you are dealing with a stubborn case of athlete’s foot or an unexplained facial rash, our specialists are equipped to deliver targeted, evidence-based care tailored to your specific situation.
South Florida’s climate creates a near-perfect environment for dermatophyte fungi. The combination of high heat, persistent humidity, and abundant access to pools, beaches, and recreational facilities means that residents face year-round exposure risk. We see athlete’s foot and its secondary manifestations throughout every season, not just summer.
For patients in Miami and surrounding areas, this makes proactive foot care more than a cosmetic concern. It is a genuine health priority. Maintaining foot hygiene, seeking early treatment, and staying informed about how fungal infections behave is directly relevant to daily life here.
Athlete’s foot is far more than a minor inconvenience confined to your feet. The dermatophyte fungi responsible for it are opportunistic, highly contagious, and entirely capable of spreading to your face through the simple act of touching your feet and then your face without washing your hands. The resulting condition — tinea faciei — is frequently misdiagnosed and can worsen significantly if treated with the wrong medications.
Recognizing the connection between foot fungal infections and facial skin changes, treating both sites simultaneously, and practicing disciplined hygiene routines are your most powerful tools. And when symptoms persist or spread, prompt evaluation by a medical professional is always the right move.

Dr. Peter Hanna is a board-certified podiatrist and reconstructive foot & ankle surgeon with over 15 years of experience. He serves as Director of Podiatry at South Florida Multispecialty Medical Group, specializing in complex reconstruction, minimally invasive surgery, and diabetic foot care.
Trust & Transparency: Editorial Policy | Contact Us
More To Explore

What Exactly Is AOD-9604? Weight loss science has come a long way from appetite suppressants and crash diets. AOD-9604 represents one of the most targeted

Most people pick up a pair of shoes based on what looks good or what is on sale and wear them for everything. Walking

©2026 South Florida Multispecialty Medical Group. All Rights Reserved.