
Types of Ankle Injuries: Sprains, Fractures & Ligament Tears
Ankle injuries are among the most common musculoskeletal problems in the United States, affecting athletes, weekend warriors, and everyday individuals alike. An estimated 25,000

Medically Reviewed by
Dr. Peter Hanna, DPM
Board Certified Podiatrist

Nearly 20 percent of U.S. adults report cracked skin on their feet, and in humid South Florida we see it surge every season once sandals come out and air conditioning dries the skin. The good news is that most heel fissures can look and feel dramatically better by morning if we follow the right nighttime protocol. At SFL Medical Group, our podiatry team treats cracked feet every week, and we built this overnight plan from what actually works in clinic.
Cracked heels, medically called heel fissures, form when the skin around the heel loses moisture, thickens into a callus and then splits under pressure. The heel pad expands every time we take a step, so once skin turns rigid it has nowhere to flex and it tears. In Miami we often see this in patients who wear flip-flops year-round, walk barefoot on tile, or stand on hard floors at work.
Common triggers we identify in our clinic include:
Most fissures are annoying but harmless. A deep crack, though, can bleed, get infected and in people with diabetes or vascular disease become an emergency. The CDC lists dry, cracked skin on the feet as a direct reason to call your doctor if you are diabetic, and our diabetic foot care team sees ulcers every month that began as ignored heel cracks.
Call a podiatrist the same week if you notice any of the following:
Our Miami podiatry clinic also evaluates for underlying causes like fungal infection, thyroid disorders and nutritional deficiencies, because treating the skin alone will not work if the root cause keeps firing.
Here is the exact nighttime routine we walk patients through. It takes about 25 minutes of active time, and then your body does the rest while you sleep. Consistency over three to five nights produces the most dramatic change, though many patients feel softer skin after a single session.

Fill a basin with warm, not hot, water. Hot water actually dehydrates skin further. Add one of the following:
Soak for 10 to 15 minutes. This hydrates the outer skin layer and softens the callus so we can safely remove dead tissue.
While skin is still damp, use a pumice stone or a foot file in small circular motions on the callused zone. Never use a razor, credo blade or sharp tool at home. We see weekly injuries from patients who did, and cutting yourself opens a direct path for bacteria. Diabetics should skip this step entirely and let us handle callus debridement in clinic.
Pat, do not rub. Then, within three minutes, apply a humectant-rich cream. Look for these active ingredients on the label:
Urea and lactic acid are humectants that pull water into the skin, while salicylic acid chemically exfoliates the callus. In clinic we reach for creams like CeraVe SA, AmLactin, Eucerin Advanced Repair and Kerasal Intensive Foot Repair.
Over the cream, spread a thin layer of petroleum jelly, Aquaphor or a plain shea butter balm. This occlusive layer traps the humectant against your skin so it can hydrate all night instead of evaporating into the Miami breeze.
Slip on clean cotton socks. Cotton breathes, prevents the cream from staining sheets and keeps a steady warm environment that boosts absorption. In the morning, your heels should feel noticeably softer and any shallow fissures should already be closing.
Patients often ask if kitchen ingredients really help. Several do, and the research backs them up when used correctly. We suggest them only for mild dryness and never as a substitute for medical care when cracks are deep.
Avoid lemon juice if the skin is already split. The acid stings and can delay healing of an open fissure, even though it helps exfoliate intact dry skin.
Not every viral hack is safe. In our Miami clinic we have treated complications from each of the following, so please skip them:
Overnight treatment is only half the battle. To keep feet smooth after the first good night, we coach patients to shift a few daily habits.
If you wake up to cracks that still bleed, sting when you walk or show any discharge, we encourage you to book a podiatry visit at SFL Medical Group. In-office treatments we offer include professional debridement of thickened skin, prescription-strength urea or keratolytic creams, custom orthotics that redistribute heel pressure, and wound care for infected or diabetic fissures.
For patients with vascular issues, our vascular surgery team evaluates circulation since poor blood flow is a leading reason heels will not heal. We also treat diabetic foot ulcers before they escalate, coordinating between podiatry, vascular surgery, and primary care all under one roof at our Miami clinic.

Recurring heel fissures that resist every home remedy often point to something deeper. Conditions such as eczema, psoriasis and athlete’s foot actively damage the skin barrier while it is trying to heal. Our dermatology and podiatry teams frequently co-manage patients whose cracked heels are a symptom of a broader skin condition. If cracking always returns within days of treatment, schedule a comprehensive foot evaluation so we can identify the root cause.
Diabetes is another major driver. High blood sugar impairs skin cell turnover and reduces moisture retention, making heels crack faster and heal slower. If you have not had a diabetic foot screening in the past year, now is the right time to book one. Early detection of neuropathy and circulation issues can prevent a simple heel fissure from becoming a non-healing wound.
A 54-year-old teacher walked into our Miami clinic last summer with bleeding heels after a weekend in sandals at the beach. She had tried three different drugstore creams with no luck. We debrided the callus, prescribed 20 percent urea cream, handed her the exact overnight routine above and switched her to a supportive sandal. Within five nights her heels closed and within three weeks she was back to smooth skin. Cases like hers are the rule, not the exception, when the protocol is followed.

Cracked feet are common, treatable and often reversible in a single night with the right combination of soak, exfoliation, humectant cream, occlusive seal and cotton socks. The key is catching them before they deepen and addressing medical causes that keep the skin dry. If you live in Miami or anywhere across South Florida and your feet are not responding to home care, our SFL Medical Group podiatrists are ready to help.

Dr. Peter Hanna is a board-certified podiatrist and reconstructive foot & ankle surgeon with over 15 years of experience. He serves as Director of Podiatry at South Florida Multispecialty Medical Group, specializing in complex reconstruction, minimally invasive surgery, and diabetic foot care.
Trust & Transparency: Editorial Policy | Contact Us
More To Explore

Ankle injuries are among the most common musculoskeletal problems in the United States, affecting athletes, weekend warriors, and everyday individuals alike. An estimated 25,000
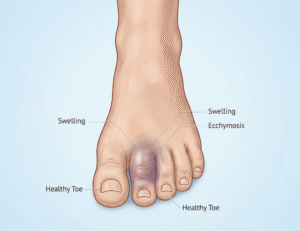
Roughly 8 to 10 percent of all fractures treated in emergency departments involve the foot and toes, yet a significant number of patients walk

©2026 South Florida Multispecialty Medical Group. All Rights Reserved.