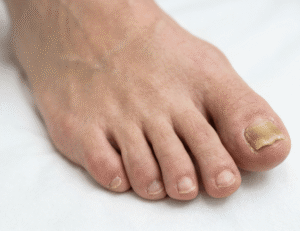
What Causes Thick Toenails? 7 Common Reasons Explained
The Nail That Shouldn’t Be Ignored Thick toenails affect millions of people, yet most of them brush off the symptom as nothing more than

Medically Reviewed by
Dr. Paul Hanna, DO, RPVI
Board Certified Vascular Surgeon

Most people assume their bodies are perfectly symmetrical. They’re not. Minor differences between the left and right sides of our bodies are completely normal. But when one leg becomes noticeably bigger than the other, especially with swelling, heaviness, pain or skin changes, that’s your body sending a signal that something deeper may be going on.
As vascular surgeons at SFL Medical Group, we evaluate patients with this exact concern regularly. More often than not, the root cause traces back to the vascular system. Blood flow problems, damaged vein valves, blood clots or lymphatic dysfunction can all make one leg swell well beyond a harmless asymmetry.
Let’s walk through what causes one leg to be bigger than the other, how we diagnose these conditions and when you should seek evaluation from a vascular specialist.
Our bodies are naturally asymmetric. One leg may carry slightly more muscle mass because it’s your dominant side. Athletes, runners and people who favor one leg during daily activities often notice a mild size difference between their thighs or calves.
In these cases, the difference tends to be subtle. There’s no sudden onset, no skin changes, no pain. Both legs feel healthy and function well. If your legs have always looked a little different with no associated symptoms, it’s likely nothing to worry about.
However, when the difference becomes noticeable over weeks or months, or appears suddenly with swelling, warmth, redness or discomfort, it’s time to get a vascular evaluation.
When we see patients with unilateral leg swelling, the vascular system is almost always the first place we look. Veins, arteries and lymphatic vessels play a direct role in regulating fluid balance in the legs.
Deep vein thrombosis is one of the most serious causes of sudden swelling in one leg. DVT occurs when a blood clot forms in a deep vein, most often in the calf or thigh. The clot blocks normal blood flow, causing fluid to back up and the leg to swell.
Patients with DVT typically describe sudden leg heaviness, tightness, warmth and sometimes redness. What makes DVT particularly dangerous is the risk of pulmonary embolism. If a clot breaks free and travels to the lungs, it can be life-threatening.
Risk factors include prolonged immobility (such as long flights or bed rest after surgery), recent surgery, cancer, pregnancy, obesity and a family history of blood clots. We confirm DVT with duplex ultrasound imaging.
Treatment starts immediately with anticoagulation therapy to prevent clot propagation. In severe cases, we may perform catheter-directed thrombolysis or mechanical thrombectomy to remove the clot. Early treatment reduces the risk of long-term complications like post-thrombotic syndrome.
CVI is one of the most common vascular conditions we treat. It develops when the valves inside leg veins stop working properly. These valves keep blood flowing upward toward the heart. When they fail, blood flows backward and pools in the lower leg.
Over time, pooling leads to persistent swelling, heaviness, aching and visible varicose veins. If CVI goes untreated, it can progress to skin discoloration around the ankles, skin thickening (lipodermatosclerosis) and eventually venous ulcers.
Treatment options range from compression stockings and leg elevation to minimally invasive procedures such as endovenous laser ablation, radiofrequency ablation or sclerotherapy.
May-Thurner Syndrome is a condition many patients have never heard of, yet it’s a significant cause of left leg swelling. It occurs when the right iliac artery compresses the left iliac vein against the spine, restricting blood flow returning from the left leg.
Chronic compression can lead to spur formation inside the vein wall, narrowing the vessel and significantly increasing DVT risk in the left leg. Diagnosis typically requires advanced imaging such as CT venography, MR venography or intravascular ultrasound (IVUS).
The most effective treatment involves venous angioplasty and stent placement to keep the compressed vein open permanently. This procedure is minimally invasive with excellent long-term results.
PTS is a chronic condition that develops after a DVT, affecting 20 to 50 percent of patients who have had a deep vein clot. The clot causes inflammation that damages vein valves and walls, leading to chronic venous hypertension.
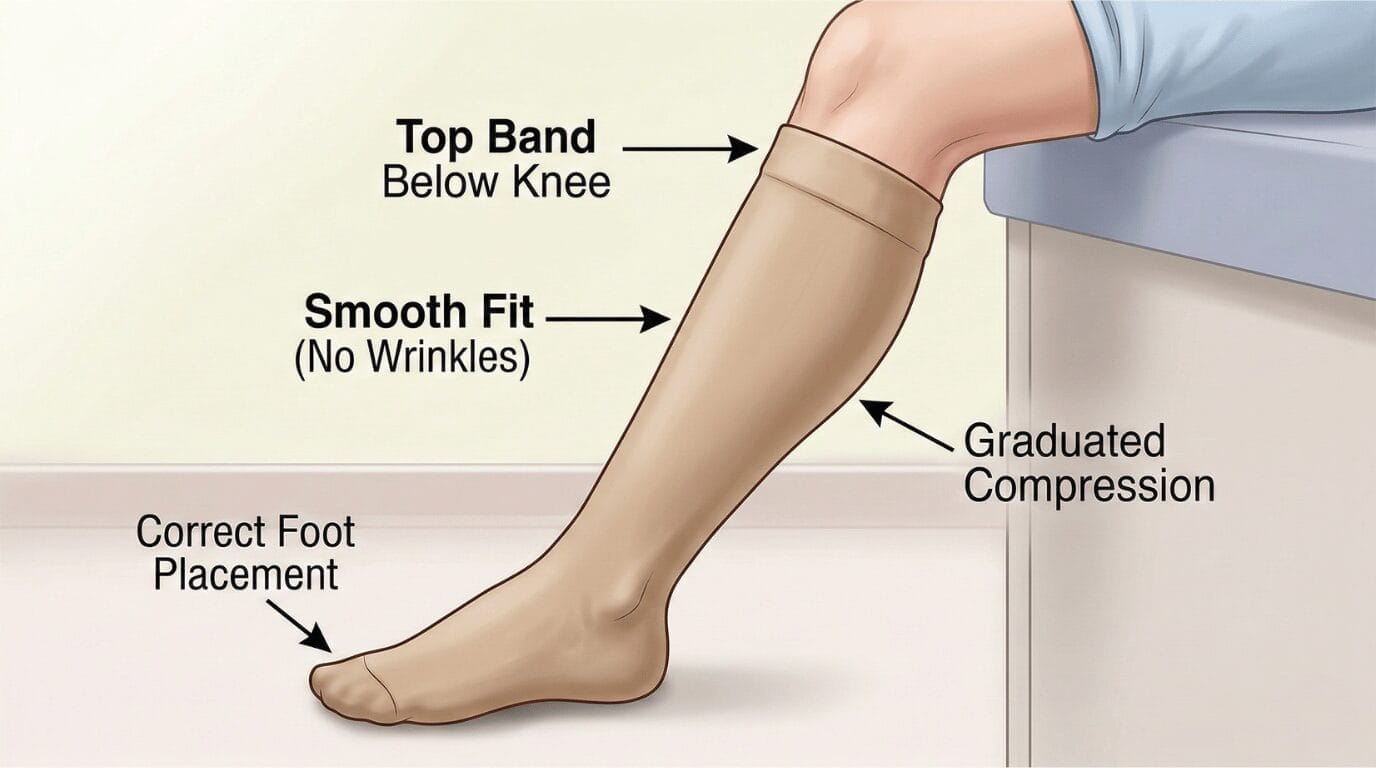
Patients experience ongoing leg swelling, pain, heaviness and skin changes. In severe cases, the leg develops permanent discoloration, tissue hardening and venous ulcers. Compression therapy is the cornerstone of treatment, using graduated compression stockings rated at 20 to 40 mmHg. For severe PTS with persistent obstruction, we perform endovascular recanalization with stent angioplasty.
Lymphedema occurs when lymphatic vessels are damaged or blocked, causing fluid to accumulate and the limb to swell. Secondary lymphedema is the most common form and typically follows cancer treatment, trauma, infection or severe chronic venous disease.
Unlike venous swelling, lymphedema tends to involve the entire limb including the foot and toes. A classic sign is a positive Stemmer sign, where the skin at the base of the second toe cannot be pinched. Treatment involves complete decongestive therapy (CDT), combining manual lymphatic drainage, compression bandaging, exercise and skin care.
At SFL Medical Group, evaluation starts with a thorough history and physical examination. We compare both legs for circumference differences, check for pitting edema, skin changes, varicose veins, warmth and tenderness.
Duplex ultrasound is our first-line imaging tool. It allows us to assess the venous system, check for blood clots, evaluate valve function and measure blood flow. For suspected central venous obstruction, we use cross-sectional imaging with CT venography or MR venography. In select cases, intravascular ultrasound (IVUS) provides the most detailed view of the vein interior.

Not every case of mild leg size difference requires a specialist visit. But certain signs demand prompt vascular evaluation. You should see a vascular surgeon if you experience:
If swelling is accompanied by chest pain, difficulty breathing or coughing up blood, that’s a medical emergency. Call 911 immediately, as these could be signs of a pulmonary embolism.
Our vascular surgery team provides a full range of treatments for conditions that cause unilateral leg swelling. We always start with the least invasive option and escalate only when necessary.
Conservative treatments include medical-grade compression stockings, leg elevation protocols, supervised exercise programs and weight management guidance.
We also coordinate closely with colleagues in oncology, primary care and wound care for comprehensive management.
Untreated DVT can lead to pulmonary embolism, a potentially fatal complication. Chronic venous insufficiency progresses to skin breakdown and venous ulcers. Post-thrombotic syndrome worsens without proper compression and follow-up. And lymphedema, once advanced, becomes irreversible.
Early intervention is always better. The sooner we identify the cause, the more effective treatment becomes and the better your long-term outcome.
If one of your legs is noticeably bigger than the other, don’t wait for the problem to worsen. We take a personalized approach to every patient, from your first consultation through treatment and follow-up. Schedule a consultation with our vascular surgery team today.

Dr. Paul Hanna is a board-certified vascular surgeon with specialized fellowship training in complex vascular interventions and minimally invasive endovascular techniques. He serves as Director of Vascular Surgery and General Surgery at South Florida Multispecialty Medical Group, with over a decade of experience treating vascular conditions affecting the limbs, aorta, and peripheral arterial system.
Trust & Transparency: Editorial Policy | Contact Us
More To Explore

The Nail That Shouldn’t Be Ignored Thick toenails affect millions of people, yet most of them brush off the symptom as nothing more than

Every year, ankle injuries send millions of people rushing to the nearest clinic or emergency room and most of them arrive with the same

©2026 South Florida Multispecialty Medical Group. All Rights Reserved.